By CAH Medical | Sichuan, China
This is a specialized medical news release concerning cervical fusion surgery and its associated risks. This article explores the issue of screw loosening—a critical component of the procedure—as well as the complexities and safety considerations inherent in this highly intricate surgery, offering a comprehensive analysis of the current clinical landscape of cervical fusion.
Ⅰ. Incidence and Clinical Impact of Cervical Fusion Screw Loosening
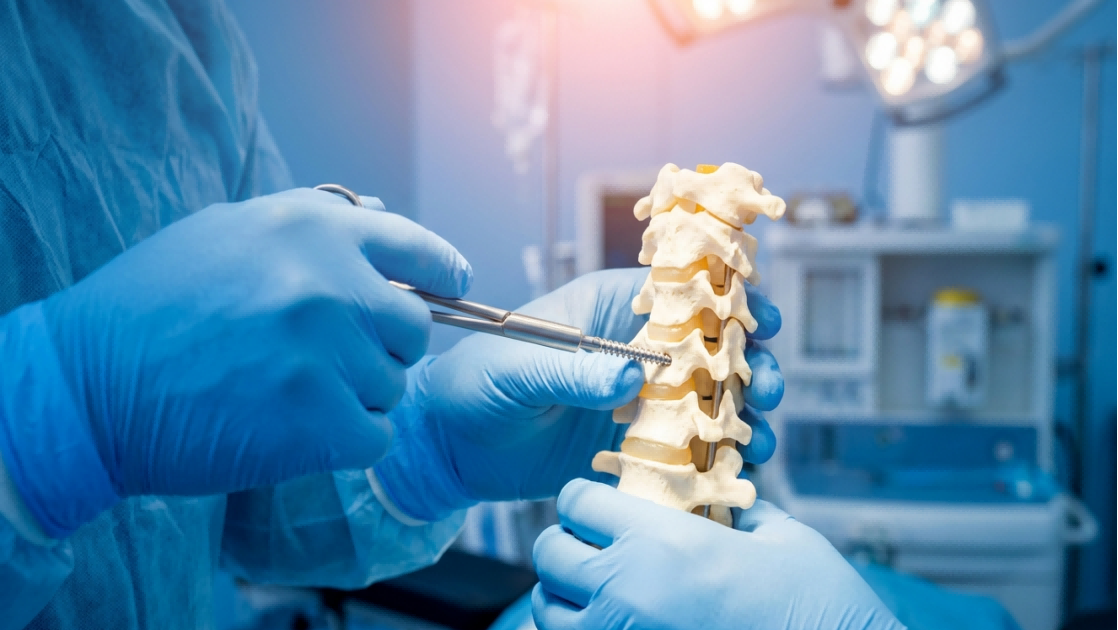
Cervical screws are core internal fixation implants used to rebuild spinal stability in cervical fusion surgery. The quality of screw fixation has a direct bearing on surgical success and long-term recovery for patients. In actual clinical work, loosening of cervical fusion screws is not a common complication. When surgeons follow standard operating procedures, place screws accurately, and carry out complete perioperative management, the chance of screw loosening stays at a low level.
Various variables impact the fixation’s stability. One is that patients that have low bone density have a low bone-screw holding power, which increases the risk of the screw loosening itself the most. A long fixation segment and early excessive neck movement after surgery. In most cases, mild loosening shows no obvious pain or dysfunction and is only found in routine imaging checks. Severe cases that need revision surgery are very rare. With careful preoperative evaluation, proper implant selection, and standardized postoperative protection, doctors can effectively improve stability and help patients achieve solid bone fusion.
Ⅱ. Cervical Spine Surgery Is a High-Grade Major Surgery
Many patients wonder if cervical spine surgery is a major surgery. According to the official surgical grading system of medical institutions, we can know that cervical fusion and internal fixation are classified as Class IV surgery, which is the most difficult and risky surgery and needs to be strictly controlled.
There are three primary reasons for this level of surgical risk. First, because of its anatomical structure, the cervical spine is in close proximity to the spinal cord, nerve roots, and cervical vertebral arteries. The surgeon has a very limited space in which to work and needs to have very precise technique to not cause injury to any of the important structures. Secondly, the procedure is complex from a technical standpoint. The patient is placed under general anesthesia and the surgical procedure consists of multiple steps that are to be completed in a sequence of nerve decompression, bone grafting, and screw placement. The surgical time to complete this procedure is relatively lengthy and requires close communication among team members and monitoring of the procedure throughout the operation. Thirdly, the postoperative care of the patient requires frequent observation of the nerve function, wound healing, and overall spinal alignment of the patient. The duration of the patient’s rehabilitation period after surgery is relatively long and requires frequent follow-up, including the professional supervision of the patient.
Surgery to the cervical spine is difficult and high level but, with the improvement in the techniques and materials used, the use of navigation system, it has become very safe. It is unusual to have complications and the clinical results are consistent and reliable. In cases where a patient has nerve compression or spinal instability, the combination of a formal cervical fusion and the use of screws will relieve the patient’s symptoms and restore the normal function of the spine so that the patient can live his/her normal daily life.
Post time: Apr-20-2026